Introduction
In Parts 1 and 2 I told the tale of how a routine scan as part of an investigation into a urinary tract infection had revealed a large (63mm) abdominal aortic aneurysm (Triple A) that needed urgent surgical intervention before it went ‘pop’ and killed me. I also described the battery of tests that I underwent in order to assess my suitability for general anaesthesia and my state of mind as the date set for the operation approached. In this thrilling episode I’ll talk about the events prior to the operation taking place, my experiences of post-operative care as an ordinary NHS patient and the start of my long and at times frustrating road to a full recovery.
For those of a nervous disposition, feel free to read this article from behind the sofa, well it worked for me with Quatermass all those years ago.
What did you mean when you said ‘it started with a piss’, Tom?
The following are not blind tasting samples of the products of a well-respected Cotswold brewery; these are genuine, non-manipulated pictures of my micturitions that started this whole business. Well, would you have been worried? It’s odd to think that they actually saved my life.

© Tom Pudding, Going Postal 2020

© Tom Pudding, Going Postal 2020
Waiting for the operation – how frustrating can it get?
The initially suggested date of January 14 for surgery had not proved to be possible so I was given the next available theatre slot of 28 January. About a week before this date I started to calm down and rationalised that in only a few days the worst would be over and all that would be left for me to do would be to get better. That’s Mrs Pudding’s philosophy regarding all things medical, but she’s much braver than I am.
The fasting information sheet from the hospital Admissions Unit stipulated that no food must be consumed after 02:00 on the day of the operation so a late evening snack was suggested to make things a bit more tolerable. Also, any regular medication that was permitted to be taken pre-op must be taken prior to 06:00 after which no liquids, not even sips of water, might be consumed. Mrs P and I arrived at the hospital at 07:15 as requested and I was then subjected to a whole range of questionnaires as part of the standard admissions procedure. I was then gowned up and visited by the anaesthetist who once again went through the procedures and risks and obtained my signature on a consent form. Next I was visited by the vascular surgeon who would be performing the operation, given an explanatory briefing and asked to sign another consent form and then it was just a matter of waiting…….and waiting……..and waiting. Then to our astonishment and great disappointment and after having been gowned for more than three hours, I was told that no ICU bed was available for me and could I come back next week? Bloody hell, that was a hard blow to take and I went home in a daze. What the hell was going on? £5.50 in wasted hospital parking charges – kerching!
So, on 05 February I went through the same fasting rigmarole, arrived at 07:15, got gowned up and after yet more blood had been taken, you guessed it, I was told that unfortunately once again no ICU bed was available and could I come back again next week? This was getting beyond a joke and, as you can imagine, my emotions were all over the place. Stunned perhaps describes best how I was feeling. My lovely surgeon lady was absolutely fuming but, despite her very best efforts, beds that do not exist cannot magically be made available – even for me. It was at this stage that I began to worry whether or not I would live long enough to have my urgently needed surgery. Another £4.40 in wasted hospital parking charges – kerching!
The next day, I received a letter from the hospital inviting me to attend at 09:30 on Tuesday 11 February. As the daily ‘bed conference’ takes place at 10:00 I realised that if I was asked to put on a gown, the operation would be going ahead yet there was still that nagging voice at the back of my mind saying, ‘I bet they cancel it again.’
This time, however, everything was much more purposeful and I was reassured that my Triple A repair would definitely be taking place that morning. After I’d put on my gown, a young and rather dour anaesthetist (the fourth I’d spoken to) came to talk me through the epidural, the only part of the procedure that really had me worried and when he saw that I was feeling a bit groggy he took me to a chair near a window for some fresh air where I did what any noble Puffin would do in the circumstances and bravely fainted. Oh, the shame. One minute I was in a chair and the next I was flat out on a trolley surrounded by a whole host of concerned looking medics and nurses.
Shortly afterwards I was wheeled into the operating theatre ante room where a lovely lady in scrubs supported and comforted me while the anaesthetist did his best to insert the epidural into my spine. I had thought that an epidural was simply an injection given to pregnant women to numb the lower extremities during the birthing process but in Triple A surgery, a needle is inserted between two vertebrae and a plastic tube is then fed into the space next to the spinal cord through which anaesthetic is fed constantly by means of a drip. The anaesthetist had four goes at it but as he wasn’t satisfied that it had gone in properly he then inserted two catheters into the Rectus Sheath (six pack) muscles as an alternative but I think this must have happened while I was asleep.
When I had my bypass 20 years ago, I distinctly remember being asked to count back from 100 but this time one minute I was awake and the next (where did the intervening four hours go?) I woke up in the ICU with no drama, no nausea, no headache – I was simply ‘there.’
So what did they do to me?
While I was unconscious and prior to surgery another large intravenous cannula was inserted into the back of my left hand for the administration of drugs and fluids; an arterial probe was inserted inside my right wrist to monitor blood pressure; a ‘central line’ catheter was inserted into the internal jugular vein in my neck and a urinary catheter was installed.
The aorta is the largest and most important artery in the human body. It is a tube normally about the size of a garden hose that runs from the left ventricle of the heart down through the chest and diaphragm close to the spine feeding oxygenated blood to the brain, heart, kidneys and other major organs before splitting into the two iliac arteries in the lower belly. The CT scan had shown that not only did I have an aortic aneurysm but that one of my iliac arteries also had a slight bulge that needed treatment.
The repair is effected by a clamping off the aorta and iliac arteries above and below the damaged section, making an incision into the bulged portion into which the trouser-shaped Dacron tube is inserted before everything is stitched back into place. It all sounds so simple but it is not without serious risks and the skill of the surgical teams that undertake this sort of work is almost beyond comprehension and very humbling. We owe them so much.
Bakerstmd / CC BY-SA
The Intensive Care and High Dependency Units
Later that Tuesday afternoon I woke up in Intensive Care where patients have 24 hour one-to-one care provided by two highly skilled nurses, one for the day and the other for the night shifts.
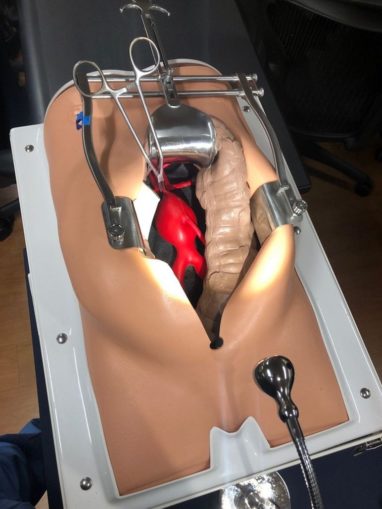
To check the effectiveness of the epidural, the nurses spray a very cold liquid onto the arm to provide a control and then they progressively spray you down your side, the theory being that if the anaesthetic drip is doing its job, the coldness will be less noticeable the lower down the body it is sprayed. Sadly for me, it all felt pretty much the same so it was clear that the epidural had been a bit of a failure. Thankfully I had been provided with a Patient-Controlled Analgesia (PCA) pump that delivered a shot of morphine direct into my jugular at the press of a button. This I christened ‘The Button of Tranquillity’ as it provided an instant feeling of well-being as and when needed. The pump (the yellow plastic box in the picture) has an interlock that prevents overdosing by locking the operating button for five minutes after each shot. I was told to use it as and when I felt I needed it and definitely before physio visits.
Perhaps the worst aspect of this period of my recovery was the constant incredibly dry mouth that resulted from the anaesthetics used during the operation. I was provided with a small sponge on a stick to dip in water and suck as required as fluid intake was being restricted.
© Tom Pudding, Going Postal 2020
The physios came to see me the morning after the operation and had me stand at the side of my bed using a Zimmer frame for support and then sit in a chair. They also had me push against them with my feet, knees and thighs and commented on my good state of general fitness, strength and the exceptionally strong pulses in my feet.
So, on the Wednesday I was moved to High Dependency where my two lovely nurses followed me but with each now being responsible for two patients rather than just one in the ICU.
Men’s Surgical
The demand for beds, especially in the ICU and HDU, is a constant problem and the next day I was moved to an ordinary ward with three other patients all of whom were diabetic. One of these was a young chap in his 30s who had gone in for a routine clinic appointment a couple of days earlier and had his left leg amputated above the knee later that same afternoon. I felt so sorry for him but he seemed very philosophical about everything and appeared to be coping in a wheelchair remarkably well, so well in fact that he disappeared with a couple of his mates one evening and went to the pub. I think he was a bit of a rogue.
One of the other old chaps seemed completely out of it and was rambling incoherently about a pair of underpants that somebody had stolen from his bag. He had had a foot removed. The other old git directly opposite me was a complete and utter arsehole. Imagine if you will a scene from a Thomas Hardy novel where a group of local ploughmen, shepherds, drovers and labourers are drinking in the pub. Chances are you wouldn’t understand a word of their conversation due to the thick Wessex accents and dialect. This idiot, who had had some toes removed, never stopped talking in such a monotonous drone that I found it impossible to understand him no matter how hard I tried. The Indian and Filipino nurses didn’t have a clue what he was saying to them and he made no effort to help them. When I had visitors he would butt into our conversations and he was constantly swearing at the foreign staff who were tending him, the ignorant pig. Incidentally, it was gratifying to learn that both of the ‘old’ chaps on the ward were in fact a few years younger than me.
A Night in Cardiology
The next evening my Indian nurse seemed puzzled that she was unable to obtain a stable blood pressure reading thinking that the monitor was faulty as it showed my pulse to be 180 plus and irregular. When I explained that my heart had gone into Atrial Fibrillation I was visited by a cardiologist who administered some drugs and had me transferred to his ward where I was monitored overnight. Everything stabilised pretty quickly and in the morning I was moved back to Men’s Surgical but this time, thank God, into a two-patient side ward with an absolutely charming man who was awaiting delivery of some sterile maggots that would be placed on his feet to eat up the corrupted flesh in an attempt to avoid amputation. What next, leeches, bleeding?
Discharge
Seven days after my operation I was taken by a couple of physiotherapists to a quiet flight of stairs where I was asked to demonstrate how well I could manage going up and down and then asked if I felt that I could walk back to my bed? No problem, so later that afternoon I was officially discharged. The ride home in my wife’s Honda Jazz was absolute agony with me feeling every bump and ripple in the road surface despite clutching a pillow to my pot belly throughout. What a relief it was to reach home.
The Long Road Back to Health
My surgeon had warned me that full recovery from this major operation will normally take from three to six months and that I should expect minor ups and downs along the way. Fortunately, I have a mate up in Yorkshire who had the same operation last year and he has been a great source of information and support over the phone since I came home.
The first and most important issue was getting the old guts working normally again after the pummelling and anaesthetics to which they had been subjected. I’ll spare you the rather unsavoury details but the moment everything snaps back to normal your whole outlook on life changes for the better.
At the time of writing (operation day plus 17) I am up and about, climbing the stairs, taking showers as normal and generally moving normally albeit slowly and with great care. I have set myself goals of walking short and gradually increasing distances each day but the weather has been so bad that so far I have only been outdoors twice.
I removed the wound dressing yesterday and now have the joy of my clothing rubbing on my wound as it heals. The surgeon closed the wound with dissolving sutures so there are no stitches or staples to worry about which is a great relief but boy, does it bloody itch!
And that’s about it. Time, they say, is a great healer so all I can do is to take things easy, let my family pamper me and not try to do too much too soon. I think I can manage that.
Conclusions and Learning Points
My surgeon told me that it is normal to experience changed organoleptic taste post-op but I wasn’t expecting to go off tea which to me now tastes bitter and metallic. Things should return to normal shortly but no one knows why this happens.
Going to the hospital Heart Club and exercising once a week for the past 18 years has kept me relatively fit, strong and mobile when compared with many of my contemporaries and this has served me well during the pre-operative and post-operative assessments. My advice would therefore be that if you are anticipating any major surgery in the near future, go out of your way to keep fit and active prior to going into hospital. A daily walk will work wonders. I suppose that I’m lucky in that although I grew up in a smoking household (everyone smoked in the 50s and 60s), I never got hooked and while I tried the occasional Woodbine out of teenage bravado, I didn’t like the taste. So far as the consultant anaesthetist was concerned, I have never smoked. The anaesthetists are very keen on measuring lung capacity and they and the physios prescribe deep breathing exercises to ensure that all of the lung surface area is being used. This minimises the risk of lung infections, especially pneumonia which is a post-operative killer, and makes expressing mucus and infection so much easier.
Having seen the unfortunate diabetics with feet that looked as if they had been frostbitten, please, if you suffer from this condition, do everything you can to control your blood sugar levels and get yourself checked out regularly. The sights I saw were really harrowing and no one should have to suffer like that.
My experiences of the NHS, apart from the two delayed operation dates which were no one’s fault, have been overwhelmingly positive. Throughout my dealings with hospital staff at all levels from porters to consultant surgeons, I have been treated with the utmost courtesy, understanding and respect by dedicated professionals and I cannot praise them highly enough. I met two lovely matrons (I didn’t realise we still had them) and both were very ‘hands-on’ in the wards. The nurses clearly loved them both and the general atmosphere on the wards was very positive, due I’m sure to the management styles of these two ladies. I am pleased to confirm that neither looked like Hattie Jacques but sadly neither did the nurses look like Barbara Windsor. Trousers and flat shoes are now de rigour and the high heels and black fully-fashioned stockings of ‘Carry on Nurse’ are just a fantasy, more’s the pity.
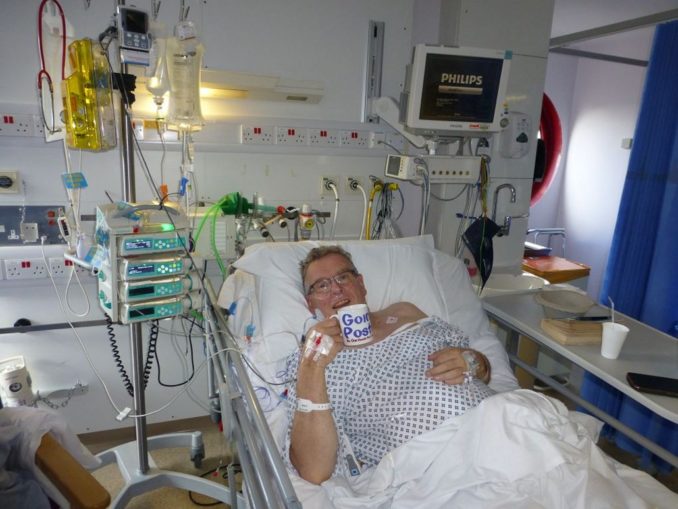
In conclusion, I would like to take this opportunity to thank all the Puffins who wished me well prior to my surgery and especially to Swiss Bob who sent my wife and me some very kind personal messages. As you can see, I took one of my GP mugs with me absolutely filled to the brim with Puffin power to help me through the difficult bits. I think it worked.
© Tom Pudding 2020
The Goodnight Vienna Audio file



