On the last Friday in July, on that stinking hot day with temperatures hitting 35, I lay recumbent in a hammock-like chair, watching the pint pour slowly. There was a gentle breeze as I counted to myself “Buttocks clench.. 1,2,3,4,5…and relax…1,2,3,4,5…..legs out 1,2,3,4,5….and in 1,2,3,4,5.”
So there I was in an NHS Blood donation centre giving my 30th pint of delicious 0 negative. It got me thinking – how did this donation thing all start and where will my blood be going to this time?
So it seems it all started just over 400 years ago (1616 in fact), with the human circulatory system – the network of arteries, capillaries and veins with the heart at its centre – being described by English physician William Harvey. Although successful blood transfusions were carried out between dogs less than 50 years later, it took until 1829 for the first successful human to human transfusion to be completed by Dr James Blundell. He took four ounces of blood from the arm of his patient’s husband using a syringe and successfully transfused it into the patient. Fortunately their blood groups were compatible because it wasn’t until 1901 that Austrian physician Dr Karl Landsteiner discovered why, when different people’s blood serum was mixed, sometimes it clotted and other times it didn’t.

Various / Public domain
From his work, Landsteiner discovered two antigens (agglutinogens A and B) and two antibodies (anti A and anti B). He called a third group C indicating the absence of both A and B antigens, but containing anti-A and anti-B. However, the path to our familiar A, B, AB and O was not smooth and a number of physicians developed their own classification systems: Czech serologist Jan Janský used Roman numerals I, II, III, and IV (corresponding to modern O, A, B, and AB) whilst American physician William L. Moss, using the same I, II, III, and IV mapped them to AB, A, B, and O. Moss’s system was adopted in Britain, France, and US, while Janský’s was preferred in most European countries and some parts of US. Confusing and dangerous!
In 1927, Landsteiner, by now a member of a committee of the National Research Council suggested substituting Janský’s and Moss’s systems with the letters O, A, B, and AB. This system was gradually accepted and by the early 1950s was universally followed.
Alongside the battle of the A, B, AB and O, Landsteiner worked with American Alexander Wiener and in 1937 they were to discover the Rh antigens, the most important of which is the D antigen. This factor can be present in our blood – making us Rh positive or absence, making us Rh negative.

Unknown (Atelier Balassa) / Public domain
So having established that, with accurate tissue typing, blood can be successfully transferred (transfused) from one person to another, Belgian doctor Albert Hustin, successfully established that sodium citrate could be used as an anticoagulant to preserve the blood and stop it from clotting outside of the body.
The first British blood bank was set up in Ipswich in 1937 and two years later, in 1939, four blood depots were established towns on the outskirts of London selected as part of war preparations to supply blood to civilian casualties as part of the newly established civilian Emergency Medical Services system. At the same time, the War Office appointed Lionel Whitby as the head of the Army Blood Transfusion Service (ABTS) based at Southmead Hospital in Bristol.
Although the ABTS and EMS exchanged blood and blood-plasma, their recruitment systems ran independently. With no direct funding from the War Office the ABTS was perhaps ahead of its time in its use of the “social media” of the late 1930s and it managed to recruit 5,000 volunteer donors to its Bristol depot using existing charities, social organisations and religious groups to spread the word. However the lack of co-ordination created many problems with volunteers responding only to be turned away by unprepared depots. The situation did improve and the ABTS’s largest recruitment drive – The Blood for Victory Campaign of February 1944 – recruited over 65,000 prospective donors through loud speaker vans, cinema adverts and radio appeals.
This poster by Abram Games OBE, R.D.I, was used by the ABTS to recruit blood donors in the early 1940s.

Creative Commons Attribution-NonCommercial-ShareAlike 4.0 Licence
In 1946 the National Blood Transfusion Service was established with the Ministry of Health taking control of blood banks. At the time, around 200,000 units of blood were collected from 270,000 donors and, in time, became more and more commonplace. Improvements were made – including the use of plastic blood bags instead of glass bottles (1975) and screening donations for HIV and hepatitis C in the 1980s.
In 1996 the regional centres of the National Blood Transfusion Service became a single, coordinated national body – the National Blood Service which, 9 years later became NHS Blood and Transplant (NHSBT) as the National Blood Service and UK Transplant merged.
Today there are 23 permanent blood donation venues in towns and cities around England with a host of temporary community-based venues setting up in church halls, sports centres, football stadiums and hotels around the country.

So going back to that day last month when I lay there watching the 470mls drip drip drip into the plastic bag, where will that blood go? Once it’s cross referenced and double checked (again!) my donation is sent to the local blood centre. The donation goes to the manufacturing area and the little test tube samples to the testing centre. In the manufacturing area, the white blood cells are filtered out and the blood is put into a centrifuge to split it into red blood cells, plasma and platelets. These are then quarantined until my test samples are completed to confirm my blood group, check for nasties and to update my donor record. Once that’s all confirmed, my blood pack is labelled and put in controlled storage, ready to be sent to hospitals at any time – day or night. Because each blood donation is split into its component parts, my one donation can help up to three people. My blood may be used to help patients with medical conditions such as anaemia or blood disorders, or will be used during surgery. My blood may also be used for research purposes or to help develop tests.
As a donor of course I won’t know who my blood has been given to but after each donation I receive a text to tell me which hospital it’s gone to and the route it took.
What do I not like about donating? Apparently I am one of only 3% of donors who don’t like the “new” plastic chairs which rock you back rather alarmingly. I’m too short to get into and out of them in anything that looks remotely elegant and they make me feel a bit sea sick – but it’s a small price to pay. And the new isotonic juice? Yeukkkk!! It’s cold drinks now – no tea – but a decent range of biscuits and crisps none the less if you’re feeling peckish afterwards.
My donation is approximately 10% of the blood in my body however that’s replaced over the next couple of weeks. The peritubular cells, located in our kidneys, are able to detect levels of oxygen in our blood. After donation, levels drop and so these cells secrete erythropoietin which passes through the bloodstream to the bone marrow and triggers an increase in production or new red blood cells. Our bodies make around 2,000,000 new red blood cells every second so it only takes a few weeks to build up stores again, at the same time drawing on our body’s reserves of iron to make haemoglobin – the protein in the red blood cells that carries the oxygen. Likewise other messenger proteins trigger the production of white cells and platelets – again by the bone marrow. Over the next few days, levels return to normal. Approximately 50% of a donation is water within the plasma. This is easily replaced with that cup of squash we drink afterwards.
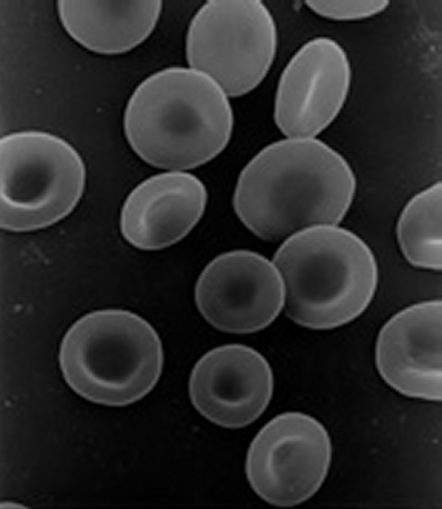
Redbloodcells.jpg: hematologistderivative work: patient-doc / Public domain
This piece isn’t an appeal for more donors – your blood is yours to do what you want with. However, there is a need for around 135,000 new donors to come forward each year to maintain the supply of essential blood and blood products needed. Today, over 1.3m people donate their “pint” – however this is a little under 2.5% of the population of England. If you’ve ever wondered about donating – take a little trip over to the website and see if you’re eligible to sign up https://www.nhsbt.nhs.uk/how-you-can-help/donate/
You don’t even have to look at the needle if you don’t want to. It’s worth it for the biscuits – just remember to take your mask at the moment.
© Hamster Wheel 2020
The Goodnight Vienna Audio file



